Knowledge of healthcare professionals about medication errors in hospitals
- *Corresponding Author:
- Dr. Mohamed M. M. Abdel-Latif
Department of Clinical and Hospital Pharmacy, College of Pharmacy, Taibah University, Al-Madinah Al-Munawwarah, Saudi Arabia.
E-mail: abdel-latif@mailcity.com
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
Abstract
Context: Medication errors are the most common types of medical errors in hospitals and leading cause of morbidity and mortality among patients. Aims: The aim of the present study was to assess the knowledge of healthcare professionals about medication errors in hospitals. Settings and Design: A self‑administered questionnaire was distributed to randomly selected healthcare professionals in eight hospitals in Madinah, Saudi Arabia. Subjects and Methods: An 18‑item survey was designed and comprised questions on demographic data, knowledge of medication errors, availability of reporting systems in hospitals, attitudes toward error reporting, causes of medication errors. Statistical Analysis Used: Data were analyzed with Statistical Package for the Social Sciences software Version 17. Results: A total of 323 of healthcare professionals completed the questionnaire with 64.6% response rate of 138 (42.72%) physicians, 34 (10.53%) pharmacists, and 151 (46.75%) nurses. A majority of the participants had a good knowledge about medication errors concept and their dangers on patients. Only 68.7% of them were aware of reporting systems in hospitals. Healthcare professionals revealed that there was no clear mechanism available for reporting of errors in most hospitals. Prescribing (46.5%) and administration (29%) errors were the main causes of errors. The most frequently encountered medication errors were anti‑hypertensives, antidiabetics, antibiotics, digoxin, and insulin. Conclusions: This study revealed differences in the awareness among healthcare professionals toward medication errors in hospitals. The poor knowledge about medication errors emphasized the urgent necessity to adopt appropriate measures to raise awareness about medication errors in Saudi hospitals.
Keywords
Error reporting system, healthcare professionals, hospitals, knowledge, medications errors
Introduction
Medication errors are the most common medical errors and under-reported in all countries, particularly in developing countries.[1-3] Medication errors may account up to one-third of all medical errors in hospital, and it can lead to adverse outcomes such as increased mortality rates, increased length of hospital stay, and high medical expenses.[4,5] Medication errors can cause serious harm to patients in several settings, particularly hospitals.[5,6] Medication errors are defined as “any preventable event that may cause or lead to an inappropriate medication use or patient harm while in the control of the healthcare professional, patient, or consumer.”[7] Morimoto et al.[8] described medication errors as errors in drug ordering, transcribing, dispensing, administering, or monitoring. The National Patient Safety Agency revealed that medication errors in all care settings in the UK occurred in each stage of the medication treatment process, with 16% in prescribing, 18% in dispensing, and 50% in administration of drugs.[9]
In all healthcare systems, medication errors are under-reported.[10-13] This under-reporting occurs in all medication use process stages: Prescribing, dispensing, and administration.[14] Under-reporting of medication errors is associated with gaps in the knowledge and wrong attitude of healthcare professionals. Other factors of under-reporting of medication errors include miscommunication, blame culture, fear of punishment, potential termination from job, and failure to comply with general policies.[15]
In a country like Saudi Arabia with multicultural background and high employment of foreign healthcare professionals in institutional and noninstitutional health sectors, the problem of medications errors and patient safety is of a great concern. It is important to evaluate their knowledge about the occurring of medication errors and reporting systems in all healthcare sectors. Alsulami et al.[16] reported that the poor knowledge of medicines was a contributory factor in both doctors (prescribers) and nurses (administering drugs) in Middle Eastern countries and indicated that educational programs for prescribers and nurses were needed to avoid drug errors and to improve patient safety. A qualitative study of challenges to medication safety in Saudi Arabia revealed that major factors contributing to reduce medication safety problems were continuous education for healthcare professionals, development of a culture that encourages medication errors reporting, use of technology proven to decrease medication errors, and promotion and implementation of national patient safety initiatives.[17]
Medical allegations usually occur from mistakes made by healthcare professionals physicians, pharmacists, and nurses.[18,19] Analyzing of malpractice claims may be used to prevent future lawsuits and improve the awareness of healthcare professionals.[20] Das et al.[21] reported that medication errors can result in malpractice claims in 13–25% of cases which occur due to mistakes and slips of action and lapses of memory. However, there is a considerable increase in awareness about the issues related to drug safety globally. In addition, the increased awareness among population regarding health matters results in increasing trends of medical practice litigations. Still, there is a lack of knowledge and incorrect perception among healthcare providers toward medication errors in healthcare institutions. Tobaiqy and Stewart[22] found that 35 respondents out of 61 participants reported observing 51 errors, and these errors caused patient harm in 14 instances in Saudi Arabia. Of the key barriers to reporting were lack of awareness of the reporting policy, workload, and time constraints associated with reporting and unavailability of the reporting form. The aim of the present study was to assess the awareness of healthcare professionals toward medication errors and assessment of the existence of reporting systems in hospitals at Al-Madinah Al-Munwwarah, Saudi Arabia.
Subjects and Methods
Study design and development of questionnaire
The study was approved by the Ethical Committee of Taibah University. The study was conducted from January 2013 to June 2013 on healthcare professionals (physicians, pharmacists, and nurses) at eight hospitals at Al-Madinah Al-Munwwarah, Saudi Arabia. A cross-sectional questionnaire was designed based on literature review, and a sample of questionnaire was tested randomly among healthcare professionals for reliability and validity, and the final questionnaire was employed for the study. The questionnaire comprised 18 questions including demographic data, knowledge of medication errors, availability of reporting systems in hospitals, knowledge of national reporting system, attitudes toward error reporting, and causes of common medication errors.
Healthcare professional’s participants
The healthcare professionals (n = 500) in hospitals were provided with a copy of the questionnaire after explanation of the objectives of the study and requested to complete the questionnaire face to face. Healthcare professional’s categories involved in the study were physicians, pharmacists, and nurses. A total of 323 out of 500 healthcare professionals participated in the study; 177 interviewers who did not return or submitted incomplete questionnaire were excluded from the study.
Statistical analysis
Complete questionnaires were collected from all participants to evaluate the response of the interviewers. Data were analyzed with Statistical Package for the Social Sciences (SPSS) software Version 17 (SPSS, Inc., Chicago, Ill, USA). Descriptive statistics were used to assess healthcare professionals’ response as mean and percent (%) of the participants. Incompleted questionnaires were excluded from the study.
Results
Demographic characteristics of healthcare professionals
A total of 323 healthcare professionals participated in the study, with a response rate of 64.6%. About 177 participants who did not return or submitted incomplete questionnaire were excluded from the study. The demographic data of the healthcare professionals’ participants are shown in Table 1. The categories of healthcare professionals were 138 (42.72%) physicians, 34 (10.53%) pharmacists, and 151 (46.75%) nurses.
| Variable | Number (% or SD) |
|---|---|
| Age | 34.65 (10.8) |
| Sex | |
| Male | 153 (47.37) |
| Female | 170 (52.63) |
| Healthcare professionals categories | |
| Physicians | 138 (42.72) |
| Pharmacists | 34 (10.53) |
| Nurses | 151 (46.73) |
| Type of hospitals (n=8) | |
| King Fahd hospital | 31 |
| Madinah Cardiac Centre | 48 |
| Ohud hospital | 47 |
| Maternity and children’s hospital | 33 |
| Prince Sultan Military hospital | 52 |
| Al Zahra hospital | 40 |
| Al Dar hospital | 34 |
| Madina National hospital | 38 |
| Nationality of healthcare professionals | |
| Saudi | 64 |
| Philippines | 108 |
| Egyptian | 97 |
| Sudanese | 32 |
| Syrian | 16 |
| Jordanians | 5 |
| Pakistani | 1 |
SD: Standard deviation
Table 1: Demographics of healthcare professionals’ participants (n=323)
Knowledge of healthcare professionals about medication errors
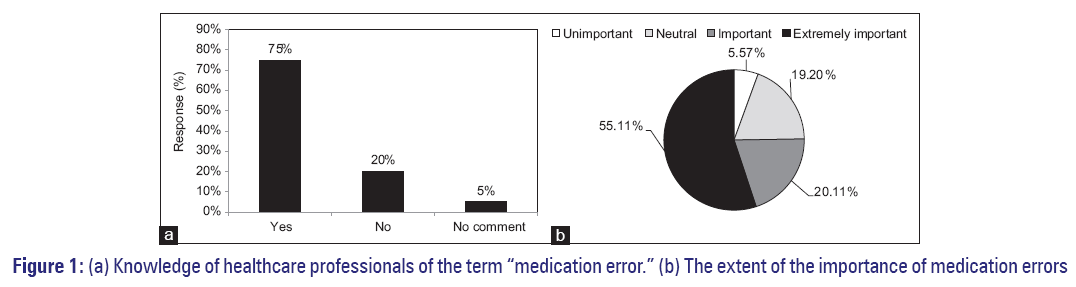
When we assessed the knowledge of the healthcare professionals about the medication error term, we noted that 74.6% of them have heard the term [Figure 1a]. In addition, among the healthcare professionals, 65% were able to define medication errors correctly and acknowledged the dangers of medication errors on patient safety and healthcare systems. We have also analyzed the knowledge of healthcare professionals about the importance of medication errors in clinical practice; we found that 55.11% of the participants considered medication errors as an extremely important problem to address it in hospitals, 20.11% as important, and 19.20% were neutral [Figure 1b]. About 5.57% of the participants thought that medication errors were not an important issue.
Knowledge of healthcare professionals about medication error reporting system in hospitals
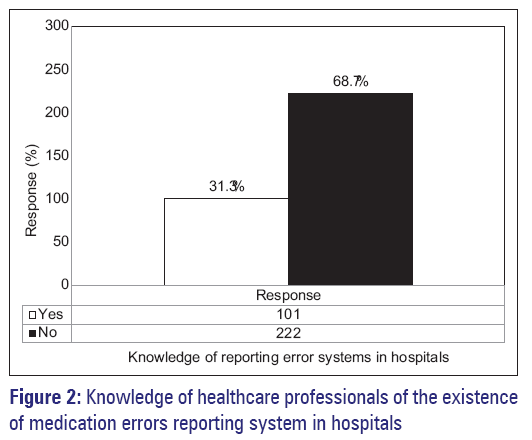
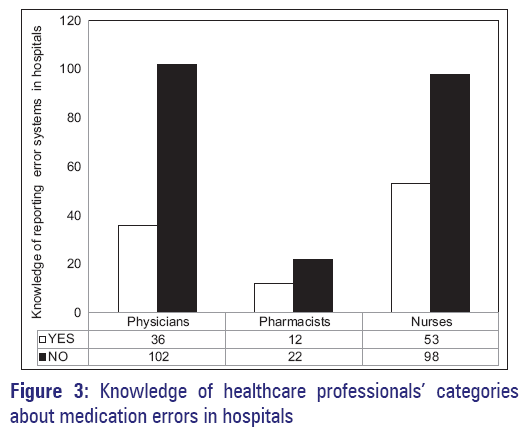
When healthcare professionals were asked about the availability of reporting system in their hospitals, only 31.3% indicated that their hospitals had reporting systems and 8.7% of healthcare professionals were knowledgeable of the existence of reporting systems in hospitals [Figure 2]. The majority of healthcare professionals were unaware of the methods of how to report the errors in hospitals. The graphical representation of the knowledge of the different healthcare professionals’ categories about medication errors in hospitals is shown in Figure 3. It shows poorer knowledge among all categories. Among 138 physicians, 73.91% had poor knowledge of the existing reporting systems in hospitals. Among 34 pharmacists, 64.71% had poor knowledge and among 151 nurses, 64.90% were found to have poor knowledge. This poor knowledge of healthcare professionals which constitutes a very high ratio, need to be addressed at those hospitals.
Attitudes of healthcare professionals to submit error reports in hospitals
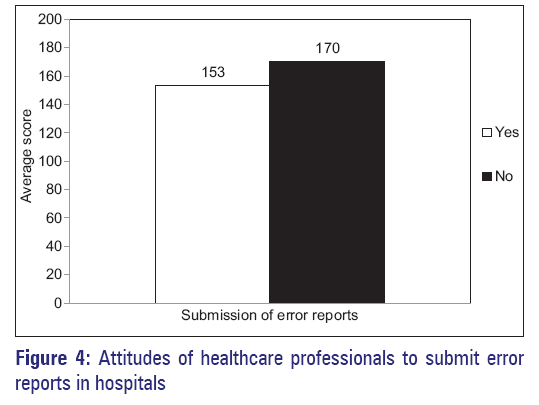
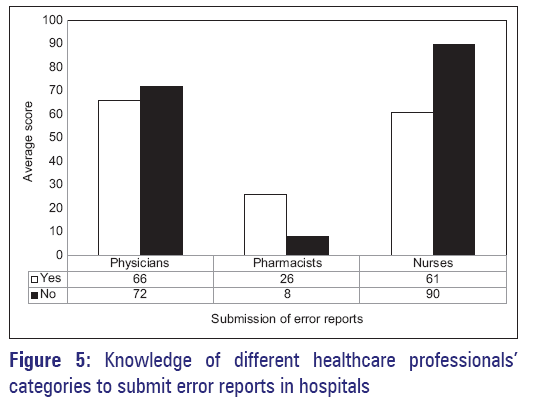
With regard to the attitudes of healthcare professionals to submit error reports in hospitals, about 47.37% of healthcare professionals were willing to submit error reports to hospital authorities [Figure 4]. The response among different categories of healthcare professionals in hospitals to submit error reports were 47.8% physicians, 76.5% pharmacists, and 40.4% nurses [Figure 5]. All the respondents agreed that they have a professional obligation and moral responsibility to report medication errors to authorities. As there was no distinct reporting system in hospitals, they stated that they did not know which medical staff/hospital authority was responsible for reporting errors in hospitals.
Causes of medication errors and common classes of drugs involved in medication errors
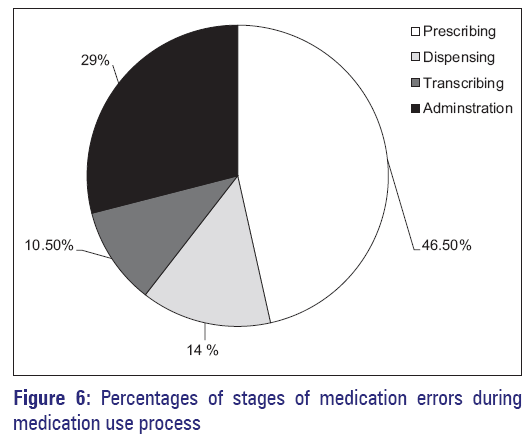
When the respondents were asked about the types of medication errors, the participants reported that most errors were caused in the prescribing and administration stages during the medication use process [Figure 6]. The proportion of medication errors was 46.5% at prescribing stage, 14% at dispensing stage, 10.5% at transcribing stage, and 29% at administration stage. The most frequently mentioned drug classes associated with medication errors were antihypertensives, antidiabetics, cardiovascular drugs, antibiotics, digoxin, and insulin.
Views of healthcare professionals of prevention of medication errors in hospitals
The most frequently mentioned suggestion among healthcare professionals for the prevention of medication errors was to report errors and introduce effective continuous medical education. Other suggestions for preventing errors were reporting mistakes, training programs and workshops, documentation of errors, introduction of electronic reporting systems, and adoption of nonblame culture in hospitals.
Discussion
The prevalence of medication errors is high even in developed countries, despite the management of medication use process using a computerized system and robotic dispensing facilities, print-out prescriptions, hospital formularies, and specialized clinical pharmacists. However, in Saudi Arabia, it is still a long way to deal with medication errors; for example, all prescriptions are still written by physicians with error-prone abbreviations and symbols, lack of good reporting systems, and a shortage of healthcare professionals. In our study, of the 500 questionnaires distributed, the response was 323 (64.6%), comprising 42.72% for physicians, 10.53% for pharmacists, and 46.75% for nurses. The present study showed a basic knowledge among healthcare professionals about the fundamentals of medication errors, but only 31.3% of the participants acknowledged that the medication errors reporting system is in place in hospitals. Of 323 healthcare professionals, about 47.37% reported errors in hospitals, but 52.63% were pointless of how and where to report errors.
We have previously demonstrated a poor knowledge and awareness of pharmacovigilance and adverse drug reactions (ADRs) reporting practice among healthcare professionals in hospitals.[23] The possible reason for the poor knowledge about error reporting systems could be due to the presence of many of the healthcare professionals of foreign nationalities who possibly did not have active pharmacovigilance reporting systems in their countries. It is clear that the major barriers for healthcare providers from not reporting medication errors were a lack of knowledge and unfamiliarity with the reporting systems and fear of reporting errors. Aljadhey et al.[24] reported that the core medication safety practices were not implemented in many Saudi Arabia hospitals and an effort is needed at the national level to increase the adoption of such practices. Only 30% of the 78 hospitals surveyed had a medication safety committee, and 9% of hospitals had a medication safety officer. Medication errors were also under-reported in a tertiary teaching hospital in Riyadh, Saudia Arabia.[25] Medication errors were reported predominantly at the prescribing stage of the medication process, and the most common types of errors were prescribing (44%) and improper dose/quantity (31%).
The main reasons for under-reporting of medication errors in our study were poor knowledge on reporting mechanisms and availability and/or accessibility of reporting systems. In agreement with these findings, several studies from different countries including UK, France, Netherland, Italy, Sweden, and others reported that there was poor knowledge of reporting systems among practitioners, and they did not know about the existence of pharmacovigilance center in hospitals.[26-30] In the European Union, many healthcare professionals did not know how to report an ADR.[31] Furthermore, about 40% of the respondents were not aware of the existence of the national reporting system in Malaysia,[32] and 71% of the healthcare professionals did not have knowledge of the reporting procedure in China.[33]
It is noted that the majority of healthcare professionals were not obliged to report medication errors in their healthcare institutions. Therefore, healthcare professionals should consider reporting of medication errors as an obligation and should be aware of the existing reporting mechanisms. Our study has revealed that many measures should be taken to curb medication errors in hospitals; such as effective communication and collaboration among healthcare professionals, development of culture of reporting errors, continuous education, frequent training workshops, and documentation of medication errors. The adoption of responsibility and nonallegation culture of medication errors reporting in hospitals could lead to the reduction of medication errors.
Medication errors can occur at any stage of the medication use process from the initial prescribing stage of a drug to its administration. The healthcare professionals revealed that prescribing errors (46.5%) and administration errors (29%) were the most frequently encountered types of medication errors in hospitals. Lesar et al.[34] stated that errors in prescribing can result from the incorrect selection of medications, wrong dose, wrong strength, wrong frequency, incorrect route of administration, inadequate instruction for use of a medication, and wrong dosage form. Furthermore, the common medication classes involved in the medication errors in our study as reported by surveyed healthcare professionals were antihypertensives, antidiabetics, cardiovascular drugs, antibiotics, digoxin, and insulin.
Conclusion
In conclusion, the present study showed that despite the awareness of healthcare professionals of the fundamentals of medication errors and their dangers on patient safety but they were unaware of the mechanics of reporting of medication errors and understand the need for the activation of reporting system in hospitals. Our findings emphasized the need for continuous education and training of healthcare professionals about medication errors and reporting errors. Our data also provide the policy makers with information for design and re-enforcement plans and educational initiatives for raising awareness among healthcare professionals toward medication errors reporting practices in hospitals. The safety practice of medications in hospitals implies that standard policies and reporting systems should be in place to foster the awareness of healthcare professionals toward medication errors and develop culture of errors reporting in hospitals.
Acknowledgements
I thank all physicians, pharmacists, and nursing staff for their participation in this study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Kohn LT, Corrigan JM, Donaldson MS, editors. To Err Is Human: Building a Safer Health System. Washington, DC: Institute of Medicine (US) Committee on Quality of Health Care in America, National Academies Press (US); 2000.
- Osborne J, Blais K, Hayes JS. Nurses’ perceptions: When is it a medication error? J Nurs Adm 1999;29:33-8.
- McLeod MC, Barber N, Franklin BD. Methodological variations and their effects on reported medication administration error rates. BMJ Qual Saf 2013;22:278-89.
- Caglar S, Henneman PL, Blank FS, Smithline HA, Henneman EA. Emergency department medication lists are not accurate. J Emerg Med 2011;40:613-6.
- Keers RN, Williams SD, Cooke J, Ashcroft DM. Prevalence and nature of medication administration errors in health care settings: A systematic review of direct observational evidence. Ann Pharmacother 2013;47:237-56.
- Benjamin DM. Reducing medication errors and increasing patient safety: Case studies in clinical pharmacology. J Clin Pharmacol 2003;43:768-83.
- National Coordinating Council for Medication Error Reporting and Prevention. What is a Medication Error? Available from: http://www. nccmerp.org/aboutmederrors.htm. [Last accessed on 2016 Mar 10].
- Morimoto T, Gandhi TK, Seger AC, Hsieh TC, Bates DW. Adverse drug events and medication errors: Detection and classification methods. Qual Saf Health Care 2004;13:306-14.
- National Patient Safety Agency. The Report from the Patient Safety Observatory. Safety in Doses: Improving the Use of Medicines in the NHS. London: NPSA; 2006.
- Allan EL, Barker KN. Fundamentals of medication error research. Am J Hosp Pharm 1990;47:555-71.
- Antonow JA, Smith AB, Silver MP. Medication error reporting: A survey of nursing staff. J Nurs Care Qual 2000;15:42-8.
- Crawford SY, Cohen MR, Tafesse E. Systems factors in the reporting of serious medication errors in hospitals. J Med Syst 2003;27:543-51.
- Mrayyan MT, Shishani K, Al-Faouri I. Rate, causes and reporting of medication errors in Jordan: Nurses’ perspectives. J Nurs Manag 2007;15:659-70.
- Hritz RW, Everly JL, Care SA. Medication error identification is a key to prevention: A performance improvement approach. J Healthc Qual 2002;24:10-7.
- Uribe CL, Schweikhart SB, Pathak DS, Dow M, Marsh GB. Perceived barriers to medical-error reporting: An exploratory investigation. J Healthc Manag 2002;47:263-79.
- Alsulami Z, Conroy S, Choonara I. Medication errors in the Middle East countries: A systematic review of the literature. Eur J Clin Pharmacol 2013;69:995-1008.
- Aljadhey H, Mahmoud MA, Hassali MA, Alrasheedy A, Alahmad A, Saleem F, et al. Challenges to and the future of medication safety in Saudi Arabia: A qualitative study. Saudi Pharm J 2014;22:326-32.
- Ruhl DS, Cable BB, Martell DW. Medication associated with hearing loss: 25 years of medical malpractice cases in the United States. Otolaryngol Head Neck Surg 2014;151:431-7.
- Madea B, Musshoff F, Preuss J. Medical negligence in drug associated deaths. Forensic Sci Int 2009;190:67-73.
- Rothschild JM, Federico FA, Gandhi TK, Kaushal R, Williams DH, Bates DW. Analysis of medication-related malpractice claims: Causes, preventability, and costs. Arch Intern Med 2002;162:2414-20.
- Das BP, Rauniar GP, Bhattacharya SK. Medical errors challenges for the health professionals: Need of pharmacovigilance to prevent. JNMA J Nepal Med Assoc 2006;45:273-8.22. Tobaiqy M, Stewart D. Exploring health professionals’ experiences of medication errors in Saudi Arabia. Int J Clin Pharm 2013;35:542-5.
- Abdel-Latif MM, Abdel-Wahab BA. Knowledge and awareness of adverse drug reactions and pharmacovigilance practices among healthcare professionals in Al-Madinah Al-Munawwarah, Kingdom of Saudi Arabia. Saudi Pharm J 2015;23:154-61.
- Aljadhey H, Alhusan A, Alburikan K, Adam M, Murray MD, Bates DW. Medication safety practices in hospitals: A national survey in Saudi Arabia. Saudi Pharm J 2013;21:159-64.
- Alshaikh M, Mayet A, Aljadhey H. Medication error reporting in a university teaching hospital in Saudi Arabia. J Patient Saf 2013;9:145-9.
- Graille V, Lapeyre-Mestre M, Montastruc JL. Drug vigilance: Opinion survey among residents of a university hospital. Therapie 1994;49:451-4.
- Cosentino M, Leoni O, Banfi F, Lecchini S, Frigo G. Attitudes to adverse drug reaction reporting by medical practitioners in a Northern Italian district. Pharmacol Res 1997;35:85-8.
- Belton KJ, Lewis SC, Payne S, Rawlins MD, Wood SM. Attitudinal survey of adverse drug reaction reporting by medical practitioners in the United Kingdom. Br J Clin Pharmacol 1995;39:223-6.
- Ekman E, Bäckström M. Attitudes among hospital physicians to the reporting of adverse drug reactions in Sweden. Eur J Clin Pharmacol 2009;65:43-6.
- Eland IA, Belton KJ, van Grootheest AC, Meiners AP, Rawlins MD, Stricker BH. Attitudinal survey of voluntary reporting of adverse drug reactions. Br J Clin Pharmacol 1999;48:623-7.
- Belton KJ. Attitude survey of adverse drug-reaction reporting by health care professionals across the European Union. The European Pharmacovigilance Research Group. Eur J Clin Pharmacol 1997;52:423-7.
- Aziz Z, Siang TC, Badarudin NS. Reporting of adverse drug reactions: Predictors of under-reporting in Malaysia. Pharmacoepidemiol Drug Saf 2007;16:223-8.
- Li Q, Zhang SM, Chen HT, Fang SP, Yu X, Liu D, et al. Awareness and attitudes of healthcare professionals in Wuhan, China to the reporting of adverse drug reactions. Chin Med J (Engl) 2004;117:856-61.
- Lesar TS, Briceland L, Stein DS. Factors related to errors in medication prescribing. JAMA 1997;277:312-7.