Drug utilization in emergency medicine department at a tertiary care teaching hospital: A prospective study
- *Corresponding Author:
- Dr. Supriya D. Malhotra
Department of Pharmacology, Smt. NHL Municipal Medical College, Ellisbridge, Ahmedabad - 380 006, Gujarat, India.
E-mail: supriyadmalhotra@gmail.com
Abstract
Background and Objectives: The practice of emergency medicine has the primary mission of evaluating, managing and providing treatment to those patients with unexpected injury or illness. Instituting appropriate therapy is necessary for safety of the patients and to decrease mortality and morbidity. The objectives were to study the drug utilization pattern and direct cost of therapy in emergency medicine department of a tertiary care teaching hospital. Materials and Methods: Data of the patients admitted to emergency medicine department was collected prospectively for 48 h from the time of admission over 2 months. The prescriptions were analyzed for drug use pattern and direct cost of therapy was calculated. Results: A total of 156 patients received 1635 drugs with the mean of 9.99 ± 2.55 drugs/patient. Most common diagnosis was acute coronary syndrome 35 (21.79%). Ondansetron 135 (86.53%) was most frequently prescribed drug followed by pantoprazole 133 (85.25%) and furosemide 68 (43.58%). Amongst antimicrobials ceftriaxone 51 (32.69%) was the most commonly prescribed drug. Direct cost of treatment per patient for the ô€ÂÂÂÂirst 48 h was र 4051 ± 1641. Conclusion: Ondansetron and pantoprazole were the most commonly prescribed drugs in the emergency department. However, their use in all patients was not justiô€ÂÂÂÂied. Polypharmacy was prevalent. A closer look at the rationality of therapy would help in highlighting issues involved and would be helpful to authorities in deciding prescribing policies.
Keywords
Acute coronary syndrome, direct cost, drug utilization, emergency medicine
Introduction
Emergency medicine is the specialty that cares for the care seeker, at the most vulnerable moments of their life. It faces the challenge of evaluating the early phases of the biological behavior in diseases. Urgency, unpredictability and the need to acquire skills of the entire spectrum of age, gender and the pathology are the hallmark of the specialty. [1] Realization of a need for better organized emergency care led to the development of emergency medicine as a specialty in the seventies in the western world. Emergency medicine is officially recognized as a specialty in nearly 50 countries around the world including India in 2009. [2,3] The problems, challenges and practices of emergency are globally similar. [4]
According to the International Federation for Emergency Medicine is a field of practice based on the knowledge and skills required for the prevention, diagnosis and management of acute and urgent aspects of illness and injury affecting patients. [5] Data from the 2002 National Hospital Ambulatory Medical Care Survey United states, showed that from 1992 to 2002, the number of emergency department visits increased from 89.8 million to 110.2 million visits annually (up by 23%). [6]
Instituting appropriate therapy is essential for a favorable outcome of the patient and to decrease mortality and morbidity. Clinicians often face challenges in selecting, initiating and individualizing appropriate drug therapy for patients admitted in the emergency medicine ward. [7] A prescription based survey (drug utilization study) is considered to be one of the most effective methods to analyze the prescribing pattern of drugs and prescribing behavior of physicians. [8,9] Monitoring the trends in drug utilization in emergency medicine can provide insight into major health-care problems. [10]
Most existing literature on emergency medicine has been brought forth from high income countries. In contrast, 70% of the population exists in low and middle income countries; hence, it is an urgent need of the hour to conduct scientifically sound well-designed study in emergency medicine with a focus on drug utilization in our country. At our institute emergency medicine as a specialty branch was recognized by Medical Council of India in 2010. Hence, this prospective cross-sectional study was undertaken with the objectives to evaluate the drug use pattern and the direct cost of treatment in patients admitted to the emergency ward for initial 48 h of hospitalization.
Materials and Methods
A prospective cross-sectional study was carried out over a period of 2 months in the emergency medicine department of our institute after obtaining approval by Institutional Review Board. All patients irrespective of age, diagnosis admitted to emergency medicine department were included in the study. Written informed consent from the patient/ legal guardian was obtained prior to conduct of the study. Patients who were very critical in the clinician’s opinion were excluded from the study. Demographic data such as patient initials, age, gender, occupation were recorded. Presenting complaints, provisional diagnosis, complete prescription and investigations were recorded in case record form for the first 48 h. Patient admitted in the emergency department of our institute were transferred to their respective specialty after 48 h of initial stabilization. Hence, data was collected for the first 48 h.
The direct cost incurred by the patient was estimated by the cost of the drug therapy, cost of investigations and days of hospital stay in the emergency ward for the first 48 h. The direct cost was calculated using hospital bills and patient’s pharmacy bills. The cost of the drugs whose pharmacy bills were inaccessible was calculated using the Indian drug review compendium-2012. [11] Confidentiality of all the patient’s data was maintained.
Statistical analyses
Data was analyzed by using Microsoft excel 2010®, Microsoft Corporation Pvt. Ltd, USA.
Results
In this study, prescriptions of 156 patients admitted in the emergency medicine department were collected for first 48 h and analysed. Majority 37 (23.71%) of patients presenting to emergency medicine department were 61-70 years of age followed by 30 (19.23%) patients with 51-60 years of age group. Male:Female ratio was 1.9:1.
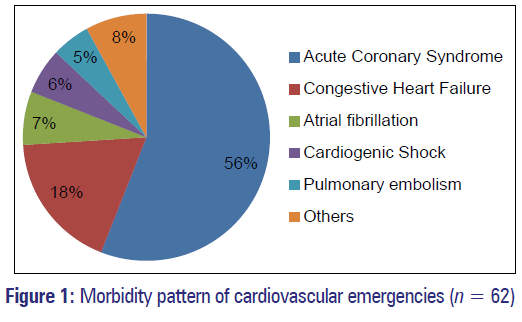
Most common morbidity was cardiovascular disease comprising 62 cases out of 156 followed by central nervous system disorders comprising of 28 cases [Table 1]. Amongst cardiovascular diseases (n = 62), acute coronary syndrome (ACS) was the most common diagnosis consisting about 35 (56%) followed by congestive heart failure 11 (17%) [Figure 1].
| Diseases | No. of patients (%) | No. of drugs/prescription (mean±SD) | Drug cost/prescription (र) (mean±SD) | Total cost/treatment (र) (mean±SD) | Cost of drugs as % of the total cost |
|---|---|---|---|---|---|
| CVS disorders | 62 (39.7) | 11.56±2.20 | 1943±1656 | 3712±1563 | 52.34 |
| CNS disorders | 28 (18.0) | 8.89±2.27 | 2315±1861 | 4725±1676 | 48.99 |
| Respiratory | 23 (14.7) | 9.22±2.76 | 2018±1281 | 3883±1690 | 51.97 |
| Metabolic | 11 (7.1) | 9.27±2.55 | 1514±1161 | 3710±1669 | 40.80 |
| Renal | 09 (5.8) | 10.22±2.90 | 2740±1429 | 4931±1818 | 55.56 |
| Others | 23 (14.7) | 10.78±2.62 | 1836±1774 | 3345±1430 | 54.88 |
| Total | 156 | 9.99±2.55 | 2061±1527 | 4051±1641 | 50.87 |
Others include cases of poisoning, snake bite, myasthenia gravis and eclampsia. SD: Standard deviation, CVS: Cyclic vomiting syndrome, CNS: Central nervous system
Table 1: Morbidity pattern, number of drugs and treatment cost in emergency medicine department (n=156)
Drug use pattern
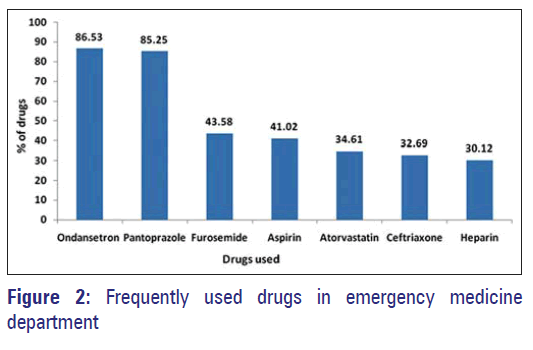
A total of 156 patients received 1635 drugs, number of drugs prescribed per patient being 9.99 ± 2.55 (mean ± standard deviation). The common drug groups used are shown in Table 2. The most frequently prescribed drugs were 5-hydroxytryptamine 3 (5-HT3) receptor antagonist ondansetron 135 (86.53%) and proton pump inhibitor (PPI) pantoprazole 133 (85.25%) followed by furosemide 68 (43.58%) [Figure 2]. Approximately, 116 (74%) of patients received antimicrobials and the third generation cephalosporin, ceftriaxone was the most commonly prescribed drug in 51 (32.69%) patients.
| Disorders (n=156) | Antiemetics | PPI | Antimicrobials | Opioids | Glucocorticoids | NSAIDs |
|---|---|---|---|---|---|---|
| CNS (n=28) | 27 | 27 | 28 | 1 | 13 | 4 |
| Respiratory (n=23) | 23 | 23 | 23 | 2 | 20 | 4 |
| Metabolic (n=11) | 11 | 6 | 11 | 4 | 0 | 0 |
| Renal (n=9) | 9 | 9 | 9 | 0 | 6 | 0 |
| Others (n=23) | 15 | 11 | 23 | 7 | 7 | 6 |
| Total | 135 | 133 | 116 | 50 | 49 | 14 |
PPI: Proton pump inhibitor, NSAIDs: Non-steroidal anti-inflammatory drugs, CVS: Cyclic vomiting syndrome, CNS: Central nervous system
Table 2: Common drug groups prescribed in various disorders
About 88% of drugs were prescribed by brand name. About 84.5% drugs belonged to national list of essential medicines India. [12] About 57.6% drugs belonged to World Health Organization model list of essential medicines. [13] Fixed dose combinations comprised 8% of total drugs.
Direct cost of treatment in 48 h
Mean cost of treatment per patient for the first 48 h was र 4051 ± 164. Mean cost of drugs per patient was र 2061 ± 1527, mean cost of investigations per patient was र 895 ± 432 and cost of hospital stay per patient was र 1100.
Discussion
Study on drug use in emergency medicine is important not only for the emergency physicians, but also for the general practitioners, who are often the first responders to emergencies in the middle and low income countries. [14] In the present study, the drug use pattern in emergency medicine department for different clinical emergencies was studied for the first 48 h.
In our study, cardiovascular emergencies were more common in males (59.68%) than in females (40.32%) and hypertension (45.16%) was the most common comorbid condition in cardiovascular emergencies in our study, which is comparable to previous Indian study carried out by Pendhari et al. on cardiovascular emergencies. [15] Hypertension is also the most common risk factor for ACS. [16]
In this study mean number of drugs per prescription, which is an important indicator of the standard of prescribing, was 9.99 ± 2.55. The reason for polypharmacy could be empirical therapy as the diagnosis may not be confirmed at the time of initial drug therapy. In an Indian study of prescribing in the emergency room, the mean number of drugs prescribed was 4.2 ± 1.2/prescription, which is in contrast to our study results. [7] This difference could be due to the fact that the patients were followed only for the duration of initial 3 h of hospital stay in the previous study. In cardiovascular emergencies the mean number of drugs per prescription was 11.56 ± 2.20, which is comparable to that reported by Pendhari et al. with the average of 9 drugs per prescription. [15] It is necessary to keep mean number of drugs as low as possible to minimise the adverse effects, potential drug-drug interactions and to reduce the cost of treatment. About 88% of drugs were prescribed by brand name as compared with study of emergency room, in which 95% of drugs were prescribed by brand names. [7] By using generic names of prescription chance of duplication of drug products is eliminated and cost to the patient decreases.
Amongst cardiovascular emergencies, ACS was most common diagnosis consisting about 56% of patients. Out of these ACS patients, 66% were ST segment elevation myocardial infarction and the rest were with non-ST segment elevation myocardial infarction/unstable angina. Streptokinase contributed to 46.92% of the total drug cost among the patients suffering from cardiovascular emergencies. The use of streptokinase was justified in all cases as it is a life-saving measure in patients suffering from ST-segment elevation myocardial infarction.
In our study, drugs acting on gastrointestinal (GI) tract, e.g. ondansetron and pantoprazole were most commonly prescribed empirically. Use of ondansetron is off-label as it is not approved anywhere for conditions other than chemotherapy or radiotherapy induced vomiting and post-operative nausea vomiting. [16] The 5-HT3 antagonists are open state blockers of the ventricular delayed rectifier and showed class III action. Ondansetron used as an off-label drug in the majority of the cardiovascular disease in our study raises concern as there are reports of higher risk of prolonged QTc interval with ondansetron. [17] However, Patanwala et al. suggested that based on the comparative safety and efficacy of ondansetron with droperidol, promethazine, prochlorperazine, metoclopramide, ondansetron may be used as a first-line agent for relief of nausea or vomiting for most patient populations in the emergency department. [18]
Physicians recommended pantoprazole a PPI as certain patients not receiving oral feeding or those receiving non-steroidal anti-inflammatory drugs, aspirin and corticosteroid are supposedly at a high risk of developing gastric mucosal damage. The most frequently mentioned explanation for prescribing PPI without an indication was “GI prophylaxis.” Jung and MacLaren suggested that PPIs are safe and efficacious for elevating intragastric pH in critically ill-patients for prevention of bleeding from stress-related mucosal damage. [19] However, a study mentioned H2-receptor antagonists as appropriate initial agents, although PPIs have become first-line therapy in an increasing percentage of critical care patients, despite limited data regarding their use in this population. [20]
Majority of the patients were inappropriately prescribed ondansetron and pantoprazole without any approved indication, which was also reported by the earlier study. [21] Ondansetron contributed to 9.2% and pantoprazole 5.8% of the total drug cost respectively. Reducing inappropriate prescribing of GI drugs in the patient minimizes potential for adverse events and fosters controllable cost expenditure. [19,22]
Approximately, 116 (74%) of patients received antimicrobials. Overestimation of the severity of illness may be the main reason for such an empirical use of antimicrobials within 48 h of admission. Antibiotic were prescribed in conditions with infective etiology use of antibiotic was justified in all cases.
Mean cost of drugs per patient for the first 48 h was र 2061 ± 1527 as compared to र 784 ± 134 in the study by Cheekavolu et al. who followed-up patients for about 3 h and hence the difference. [7]
This study was carried out for first 48 h of patient’s admission to emergency medicine department. As most of the patient’s condition stabilise in 48 h they were transferred to the respective wards for further treatment. Therefore, follow-up was restricted to 48 h. We did not estimate indirect cost like transport and other intangible costs, which if calculated will provide us more realistic picture of the financial burden to the patient. This study was first of its kind in India to our knowledge.
Conclusion
During the mean stay of 48 h in emergency medicine department ondansetron and pantoprazole usage was high. Use of these drugs in all patients was not justified and it increases the cost of therapy. Rationality of their use needs to be systematically evaluated. Polypharmacy was prevalent. The recognition of emergency medicine as a specialty is relatively recent in most countries including India. Rationalization of drug therapy in emergency medicine would be useful in managing the broad array of conditions that present for emergency care.
Acknowledgments
We are very grateful to Dr. Pankaj R. Patel, Dean of Smt. N.H.L. M.M.C who allowed us to complete this study.
References
- Tintinalli JE, Stapczynski JS, Cline DM, Ma OJ, Cydulka RK, Meckler GD. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 7th ed. North Corolina, USA: McGraw-Hill Publishing House; 2011.
- Das AK, Gupta SB, Joshi SR, Aggarwal P, Murmu LR, Bhoi S, et al. White paper on academic emergency medicine in India: INDO-US Joint Working Group (JWG). J Assoc Physicians India 2008;56:789-98.
- Decker WW, Stead LG. The international journal of emergency medicine: A new journal for a new era. Int J Emerg Med 2008;1:1-2.
- Anderson P, Petrino R, Halpern P, Tintinalli J. The globalization of emergency medicine and its importance for public health. Bull World Health Organ 2006;84:835-9.
- Suter RE. Emergency medicine in the United States: A systemic review. World J Emerg Med 2012;3:5-10.
- McCaig LF, Burt CW. National hospital ambulatory medical care survey: 2002 emergency department summary. Adv Data 2004;340:1-34.
- Cheekavolu C, Pathapati RM, Babasaheb Laxmansingh K, Saginela SK, Makineedi VP, Siddalingappa, et al. Evaluation of drug utilization patterns during initial treatment in the emergency room: A retroprospective pharmacoepidemiological study. ISRN Pharmacol 2011;2011:261585.
- Tiwari H, Kumar A, Kulkarni SK. Prescription monitoring of anti-hypertensive drug utilisation at the Punjab University health centre in India. Singapore Med J 2004;45:117-20.
- Sharif S, Al-Shaqra M, Hajjar H, Shamout A, Wess L. Patterns of drug prescribing in a hospital in Dubai, United Arab emirates. Libyan J Med 2008;3:10-2.
- Slobodan MJ, Slavica M, Dukic DJ. Drug utilization trends in clinical hospital centre ‘Kragujevac’ from 1997-1999. Indian J Pharmacol 2001;33:29-36.
- Malik A, Malik S. Indian drug review compendium. 1st ed. India: Mediworld Publications; 2012.
- National List of Essential Medicines India, 2011. Available from: cdsco.nic.in/National List of Essential Medicine- fi nal copy.pdf. [Last accessed on 2013 Aug 27].
- WHO Model List of Essential Medicines, 17th List, 2011. Available from: www.who.int/medicines/publications/essentialmedicines/ Updated_sixteenth_adult_list_en.pdf. [Last accessed on 2013 Aug 27].
- David S. Textbook of Emergency Medicine. 1st ed. India: Lippincott Williams and Wilkins; 2011. p. 1155-6.
- Pendhari SR, Chaudhari DR, Burute SR, Bite BM. A study on the drug utilization trends in the cardiovascular emergencies in a tertiary care hospital. J Clin Diagn Res 2013;7:666-70.
- Longo DL, Fauci AS, Kasper DL, Hauser SL, Jameson JL, Loscalzo J. Harrison’s Principles of Internal Medicine. 18th ed., Vol. 2. Ch. 39, 247. USA: McGraw-Hill Companies; 2012.
- de Lorenzi FG, Bridal TR, Spinelli W. Block of the delayed rectifi er current (IK) by the 5-HT3 antagonists ondansetron and granisetron in feline ventricular myocytes. Br J Pharmacol 1994;113:527-35.
- Patanwala AE, Amini R, Hays DP, Rosen P. Antiemetic therapy for nausea and vomiting in the emergency department. J Emerg Med 2010;39:330-6.
- Jung R, MacLaren R. Proton-pump inhibitors for stress ulcer prophylaxis in critically ill patients. Ann Pharmacother 2002;36:1929-37.
- Daley RJ, Rebuck JA, Welage LS, Rogers FB. Prevention of stress ulceration: Current trends in critical care. Crit Care Med 2004;32:2008-13.
- Lat I, Micek S, Janzen J, Cohen H, Olsen K, Haas C. Off-label medication use in adult critical care patients. J Crit Care 2011;26:89-94.
- Heidelbaugh JJ, Kim AH, Chang R, Walker PC. Overutilization of proton-pump inhibitors: What the clinician needs to know. Therap Adv Gastroenterol 2012;5:219-32.