Assessment of Parkinsonian Symptoms and Toxin Exposures in Firefighters
2 Department of Medicine, Tufts University School of Medicine, Boston, MA, USA
Received: 20-May-2022, Manuscript No. Jbclinphar-22-64353; Editor assigned: 23-May-2022, Pre QC No. Jbclinphar-22-64353(PQ); Reviewed: 10-Jun-2022 QC No. Jbclinphar-22-64353; Revised: 21-Jun-2022, Manuscript No. Jbclinphar-22-64353(R); Published: 29-Jun-2022, DOI: 10.37532/0976- 0113.13(3).172
Citation: Kotwani R, Clapp AN, Huggins HE, et al. Assessment of Parkinsonian Symptoms and Toxin Exposures in Firefighters. J Basic Clin Pharma 2022;13(3):172-177.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@jbclinpharm.org
Abstract
Background: Parkinson’s Disease (PD) has been correlated with several environmental and toxic exposures. The frequency of PD in firefighters is higher than the general population, which may be due to the high amounts of toxin exposures firefighters experience on the job. There is a need to further address the high rates of PD among this subgroup. The purpose of this study is to improve our understanding of the relationship between toxin exposure in firefighters and Parkinsonian symptoms.
Methods: An anonymous survey distributed to Massachusetts firefighters assessed risk factors for toxin exposure and presence of Parkinsonian symptoms. Risk factors included frequency and duration of time spent firefighting, number of fires worked, and history of toxin exposure other than from fires (i.e., pesticides). We collected the frequency of Parkinsonian symptoms including tremors, muscle stiffness, REM behavior disorder, hyposmia, micrographia, and decreased walking pace. Analyses comparing all toxin exposure and presence of Parkinsonian symptoms were performed using Chi-square testing; p<0.05 was considered significant.
Results: Two hundred participants were included in the study. The number of years as a firefighter, the number of days per week working, and the number of fires worked correlated with higher reports of hyposmia, micrographia, and decreased walking pace. Exposure to pesticides and the Vietnam war correlated with higher reports of decreased walking pace and micrographia.
Conclusion: The risk of Parkinsonian symptoms was positively correlated with exposure to several toxins associated with the work of firefighters.
Keywords
Parkinson disease, Firefighters, Environmental exposure, Toxins, Micrographia, Decreased walking pace, Hyposmia, Pesticides
Introduction
In 1986, a fire lasting five days broke out in a junkyard in Spencer, MA, burning approximately seven hundred thousand to one million tires and requiring firefighters from ten different stations to control the blaze. Ultimately, five individuals, including four firefighters, who were involved in the Spencer fire developed Parkinson’s Disease (PD) or Parkinsonism. Firefighters with their numerous toxic exposures are hypothesized to be more likely to develop Parkinson’s disease symptoms [1]. Parkinson’s disease is the second most common neurodegenerative disorder in America affecting 1% of the population age 60 or over [2]. PD is characterized by tremors, rigidity, bradykinesia, and gait disturbances. Non-motor symptoms such as hyposmia, micrographia, and REM behavior disorder may precede PD by several years [3]. These nonmotor symptoms are not specific to PD; they are seen in Parkinsonism, a group of neurological disorders associated with slowness, stiffness, difficulty walking, and occasionally tremors. Although the cause of PD has not been determined, researchers have identified several factors to be associated with the disease, including genetic, environmental, and toxic components. Prior studies have detailed five neurotoxic compounds associated with PD, including lead, styrene or vinyl benzene, benzopyrene, Polybrominated diphenyl ether, and carbon monoxide [4-12].The frequency of PD in firefighters is extremely high (1/30 people) compared to the general population (1/100 people over age 60), which may be due to the high amounts of toxin exposures firefighters experience [2,4].
Firefighters experience heavy lead exposures as they encounter buildings heavily coated with lead-based paints and spotted with lead-comprised dust [5]. Lead exposure has shown to result in a twofold increase in the risk for developing PD as it damages neurological pathways by inhibiting reuptake of calcium and decreasing the quantity of dopamine within vesicles [5,6]. Styrene or vinyl benzene is a crucial toxin encountered during fires which has been shown to alter dopamine receptor functioning and damage central and peripheral nervous systems [7].
Benzo pyrene has been shown to decrease dopamine neurotransmitter regeneration in the nucleus accumbens and hippocampus of rats [8]. A prior study that found benzopyrene on fire jackets, personal protective equipment of firefighters as well as other tools determined that current equipment cleaning standards do not eliminate benzopyrene contamination [9].
Poly Brominated Diphenyl Ether (PBDE) is a neurotoxin used in flame-retardants and found in carpets, cushions, and home-insulating structures frequently handled by firefighters [10]. PBDE uses oxidative damage to inhibit dopamine transporters DAT and VMAT2 [4]. Many studies have established the correlation between Carbon Monoxide (CO) exposure and risk of PD [11,12].
Firefighters are exposed to several environmental toxins that increase their risk of PD and there is a need to draw attention to PD among this subgroup. This study utilized a retrospective analysis based on a survey assessing the incidence of environmental toxin exposure and Parkinsonian symptoms among firefighters.
Methodology
An anonymous online survey was distributed to firefighters >18 years of age between January 2020 and August 2020 to the Professional Firefighters of Massachusetts. Demographic data collected included sex, age, race, and employment status (working, retired, volunteer, or family member of deceased firefighter). Risk factors for toxin exposure were assessed by frequency and duration of time spent firefighting and use of protective gear. A history of toxin exposure unrelated to firefighting was evaluated including prior work as a welder, consumption of well water, duration of military service, as well as exposure to Agent Orange, pesticides, and jet fuel. The presence and frequency of Parkinsonian symptoms were collected, including tremors, muscle stiffness, REM behavior disorder (i.e., acting out dreams, talking during sleep), hyposmia, micrographia, and decreased walking pace. Analyses comparing toxin exposure and presence of Parkinsonian symptoms were performed using Chi-square testing (p<0.05 was considered significant). This study was approved by the St. Elizabeth institutional review committee (IRB #EX064) and participants were provided written informed consent to participate in the study.
Results
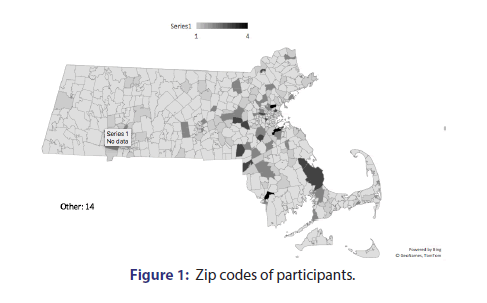
Two hundred participants were included in the study. Among participants, 96% were male, 99% were Caucasian and 1% Hispanic, 62% were still employed, 37% retired, and 12% had a family history of Parkinson’s disease (Table 1). The communities of survey participants were showed in Figure 1. The majority of our survey participants live in rural and suburban communities in Massachusetts with a few living outside the state.
| Characteristics | Number of participants |
|---|---|
| Total | 200 |
| Sex | |
| Male | 192 (96%) |
| Age | |
| 18-30 | 6 (3%) |
| 30-40 | 28 (14%) |
| 40-50 | 84 (42%) |
| 60-70 | 60 (30%) |
| 70-80 | 16 (8%) |
| Race | |
| Caucasian | 192 (99%) |
| Hispanic | 2 (1%) |
| Employment status | |
| Working | 123 (62%) |
| Retired | 74 (37%) |
| Volunteer | 3 (1%) |
| Family history of PD | 25 (12%) |
Table 1 : Participant demographics.
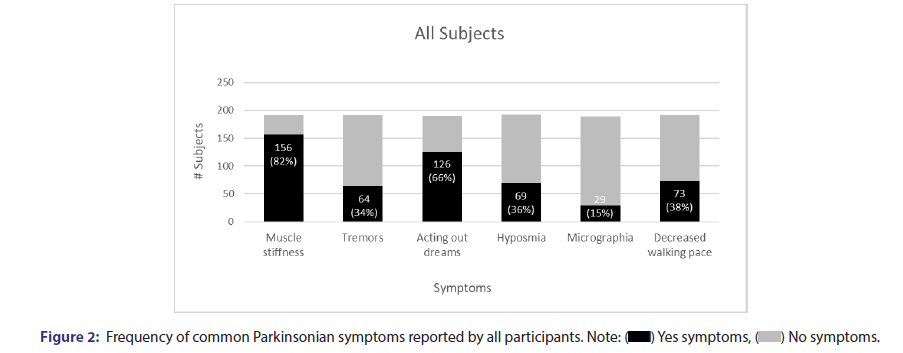
The frequency of common Parkinsonian symptoms reported by all participants demonstrated in Figure 2. 82% of survey participants reported muscle stiffness, 34% tremors, 66% REM behavior disorder, 36% hyposmia, 15% micrographia, and 38% of participants reported decreased walking pace.
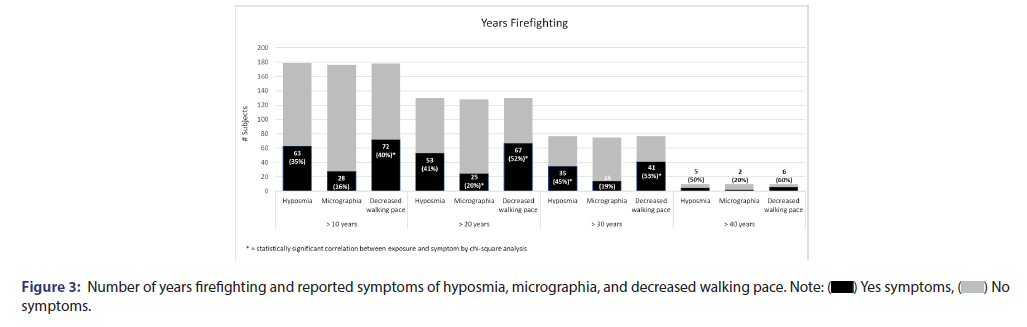
The correlation of the number of years of being a firefighter with decreased walking pace, micrographia, and hyposmia was showed in Table 2 and Figure 3. After 10 years of firefighting, participants were found to be 5 times more likely to have decreased walking pace. After 20 years, participants were 30 times more likely to have decreased walking pace and 5 times more likely to have micrographia. After 30 years, participants were twelve times more likely to have decreased walking pace and 5 times more likely to have hyposmia.
| Total | Decreased walking pace | Micrographia | Hyposmia | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 73(38%) | 29 (15%) | 69 (36%) | |||||||||||
| Exposed | Not exposed | χ2 | Exposed | Not exposed | χ2 | Exposed | Not exposed | χ2 | |||||
| Years fire fighting | |||||||||||||
| >10 years | 72 (41%) | 1 (8%) | χ2 = 4.90, P-value 0.03* | 28(16%) | 1 (8%) | χ2 = 0.49, P-value 0.48 | 63 (35%) | 6 (50%) | χ2 = 1.07, P-value 0.30 | ||||
| >20 years | 67 (52%) | 6 (10%) | χ2 = 29.94, P-value <0.001* | 25 (20%) | 4(7%) | χ2 = 5.18, P-value 0.02* | 53 (41%) | 16 (26%) | χ2= 3.8, P-value 0.05 | ||||
| >30 years | 41 (53%) | 32(28%) | χ2 = 12.03, P-value <0.001* | 14 (19%) | 15(13%) | χ2 = 1.00, P-value 0.32 | 35 (83%) | 34 (30%) | χ2 = 4.87, P-value 0.03* | ||||
| >40 years | 6 (60%) | 67(37%) | χ2 = 2.08, P-value 0.15 | 2 (20%) | 27(15%) | χ2= 0.17, P-value 0.68 | 5 (50%) | 64 (35%) | χ2= 0.88, P-value 0.35 | ||||
| Days/week worked | |||||||||||||
| ˃1 day | 46 (29%) | 26 (84%) | χ2 = 32.95, P-value <0.001* | 19(12%) | 10 (32%) | χ2 = 7.96, P-value 0.005* | 54 (34%) | 15 (48%) | χ2 = 2.41, P-value 0.12 | ||||
| >2 days | 45 (29%) | 27 (82%) | χ2 = 32.41, P-value <0.001* | 18(12%) | 11 (33%) | χ2 = 9.72, P-value 0.002* | 53 (34%) | 16 (48%) | χ2 = 2.64, P-value 0.1 | ||||
| >3 days | 36 (32%) | 36(46%) | χ2 = 3.66, P-value 0.06 | 15(14%) | 14(18%) | χ2= 0.61, P-value 0.44 | 34 (30%) | 35 (32%) | χ2 = 3.9, P-value 0.05* | ||||
| >4 days | 33 (36%) | 39 (40%) | χ2 = 0.25, P-value 0.62 | 14(16%) | 15 (16%) | χ2 = 0.0003, P-value is 0.99 | 30 (33%) | 39 (39%) | χ2 = 0.95, P-value 0.33 | ||||
| > 5 days | 21 (39%) | 51 (38%) | χ2 = 0.02, P-value 0.89 | 11(21%) | 18(13%) | χ2 = 1.55, P-value 0.21 | 18 (33%) | 51 (38%) | χ2 = 0.39, P-value 0.53 | ||||
| > 6 days | 5 (42%) | 67 (38%) | χ2 = 0.07, P-value 0.79 | 5 (42%) | 24(14%) | χ2 = 6.70, P-value 0.01* | 3 (23%) | 66 (37%) | χ2 = 1.03, P-value 0.31 | ||||
| Number of 5-9 alarm fires | |||||||||||||
| 20 or more | 18 (60%) | 50 (33%) | χ2 = 7.56, P-value <0.05* | 12(41%) | 16 (11%) | χ2 = 17.19, P-value <0.001* | 13 (43%) | 53 (35%) | χ2 = 0.73, P-value 0.39 | ||||
| 40 or more | 8 (67%) | 60 (36%) | χ2= 4.56, P-value 0.03* | 5 (42%) | 23 (14%) | χ2 = 6.53, P-value 0.01* | 7 (70%) | 59 (35%) | χ2 = 5.14, P-value 0.02* | ||||
| 100+ | 4 (57%) | 64 (37%) | χ2 =1.16,P-value 0.28 | 3 (43%) | 25(15%) | χ22= 4.04, P-value 0.04* | 4 (57%) | 62 (36%) | χ2 = 1.34, P-value 0.25 | ||||
| Vietnam war | 7 (88%) | 13 (41%) | χ2 = 5.63, P-value 0.02* | 3 (38%) | 2 (6%) | χ2= 5.71, P-value 0.02* | 4 (50%) | 11 (34%) | χ2 = 0.67, P-value 0.41 | ||||
| Pesticides | 30 (53%) | 37 (32%) | χ2 = 6.71, P-value 0.01* | 17 (30%) | 12 (11%) | χ2=10.44, P-value 0.001* | 26 (45%) | 39 (34%) | χ2= 1.96, P-value 0.16 | ||||
Note: * =statistically significant value with p<0.05 considered to be significant.
Table 2 : Parkinsonian symptoms of decreased walking pace, micrographia, and hyposmia correlated with exposures using Chi-square analysis.
The correlation of number of days per week working as a firefighter with decreased walking pace, micrographia, and hyposmia was showed in Table 2 and Figure 4. Participants were thirty-three times more likely to have decreased walking pace if they had worked more than 2 days per week. Participants were eight times more likely to have micrographia if they had worked more than 1 day per week. They were ten times more likely to have micrographia if they had worked more than 2 days per week. Participants working more than 6 days per week were seven times more likely to have micrographia.
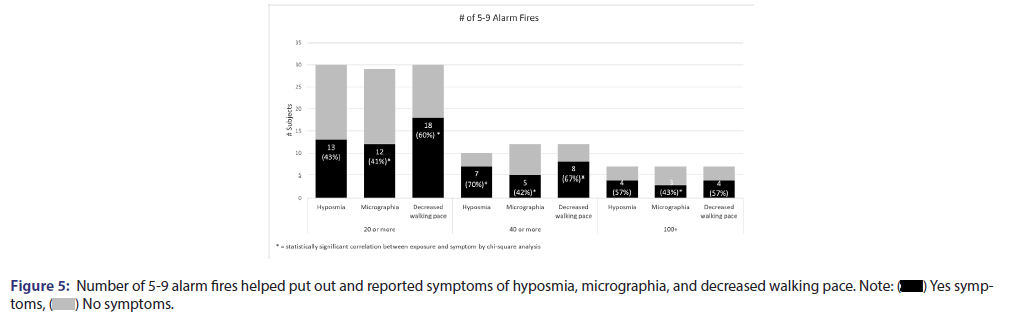
Using Chi-square analysis, the correlation between the numbers of 5-9 alarms fires worked and decreased walking pace, micrographia, and hyposmia was showed in Table 2 and Figure 5. Fire alarms are categorized based on the severity of the fire with 5-9 fire alarms being more severe. Participants who helped with 20 or more fires were eight times more likely to have decreased walking pace and seventeen times more likely to have micrographia. Participants who have helped with 40 or more fires were five times more likely to have decreased walking pace, seven times more likely to have micrographia, and five times more likely to have hyposmia. Participants who have helped with 100 or more fires were four times more likely to have micrographia.
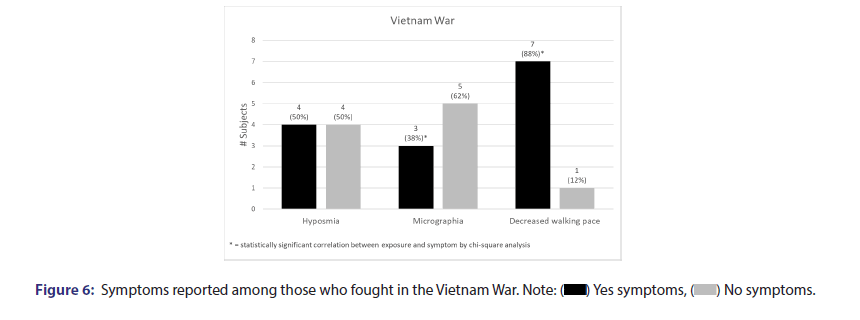
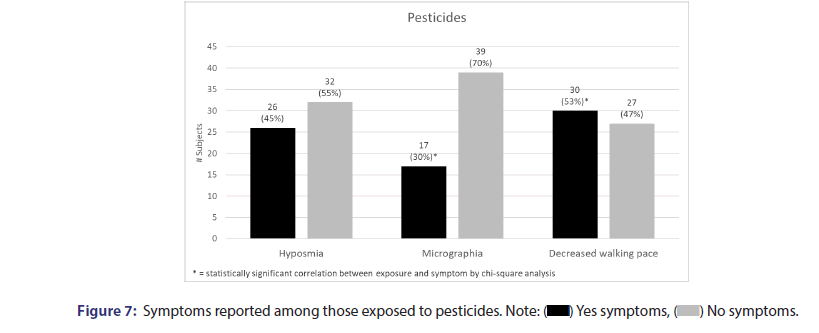
The correlation of the fighting in Vietnam War with decreased walking pace, micrographia, and hyposmia was showed in Table 2 and Figure 6. Participants who fought in the Vietnam war were six times more likely to have decreased walking pace and six times more likely to have micrographia. The correlation of exposure to pesticides with decreased walking pace, micrographia, and hyposmia. Participants who have been exposed to pesticides were seven times more likely to have decreased walking pace and ten times more likely to have micrographia was showed in Table 2 and Figure 7.
Acting out dreams was reported by 66% of survey responders. This frequency was distinctly higher than other studies which have noted REM behavior disorder in only one third of Parkinson’s patients [13]. Decreased walking pace and bradykinesia were reported by 38% of respondents. Hyposmia and tremors were the fourth and fifth most reported Parkinsonian symptoms at 36% and 34% respectively. Lastly, micrographia occurred in 15% of responders.
Discussion
After conducting a thorough literature search, we identified the five common toxin exposures in fires that have been shown to increase risk for PD. Through comparative analysis, we found that the number of years firefighting, number of days per week firefighting, number of 5-9 alarm fires encountered, fighting in the Vietnam War, and exposure to pesticides all correlated with a significantly higher frequency of three Parkinsonian symptoms: micrographia, hyposmia, and decreased walking pace.
The number of years spent firefighting was broken down into 4 categories: 10 years or more, 20 years or more, 30 years or more, and 40 years or more. It is important to note that there was a small number of survey responders who had or have been firefighting for more than 40 years (n=13). Nonetheless, the frequency of reported hyposmia and decreases in walking pace increased by an average of 5% and 7% per 10 years respectively. Meanwhile, the frequency of reported micrographia remained relatively unchanged. The duration of a firefighter’s career has also been found to positively correlate with levels of epigenetic changes, namely hypomethylation, that could lead to developments of neurodegenerative diseases [14]. Alternatively, for the number of days worked per week, the frequency of reported micrographia and walking pace increased by 6% and 3% per day, respectively.
The comparative data for the number of 5-9 alarm fires proved more difficult to gather due to the rarity of such alarm fires with only 30 being reported in Boston within the past 10 years [15]. The frequency of micrographia increased by 1% per 20 5-9 alarm fires.
It was interesting to note that muscle stiffness was the most commonly reported symptom occurring in 82% of our survey responders. Several studies have discovered elevated baseline muscle pain in firefighters [16]. Dr. Park and his team found that muscle pain was the second most common reported symptom amongst firefighters likely due to heavy personal protective equipment [17]. Thus, the muscle stiffness experienced by responders may be linked to the demands of their job or early symptoms of Parkinsonism.
Another key finding was that participation in the Vietnam War, which involved the toxin Agent Orange, was significantly correlated with decreased walking pace and micrographia. Those exposed to the Vietnam war more frequently reported decreased walking pace (88% vs. 41%), micrographia (38% vs. 6%), and hyposmia (50% vs. 34%). A number of different case studies on Vietnam war veterans have suggested that exposure to Agent Orange, specifically its 2,4-Dichlorophenoxyacetic acid component, can significantly increase the risk of Parkinson’s Disease [18].
Exposure to pesticides was significantly correlated with reported frequencies of decreased walking pace (53% vs. 32%), micrographia (30% vs. 11%), and hyposmia (45% vs. 34%). These trends align with previously conducted research which has found several pesticides and herbicides that are linked to increased susceptibilities to Parkinson’s disease. For example, one study with mice models showed that exposure to the herbicides Maneb and Paraquat can lead to mutations in genes responsible for neurogenesis which can in turn impact the development of PD [19]. Additionally, one notably deleterious pesticide, rotenone, has been shown to induce oxidative damage in dopaminergic regions of several rats [20].
Although this study provides ample data to help us understand the risks associated with firefighting, there were some limitations. The advertisement for this survey stated that the study’s aim was to determine the link between firefighting and Parkinson’s disease. This may have increased the response rate of those concerned about or affected by Parkinson’s disease. Additionally, some of the symptoms we aimed to evaluate, namely decreased walking pace, were difficult to interpret via survey. While this study had a relatively small sample size, the demographics appear to represent the typical firefighters in Massachusetts. The demographics of the sample were 96% being male, 99% Caucasian, and 72% being between the ages of 40 and 70.
Another limitation was the lack of genetic studies conducted on respondents which could have indicated possible genetic predispositions to PD or Parkinsonism. Hyposmia was reported by 36% of study participants. It is probable that the actual frequency of hyposmia is more than what was reported as this sensory symptom can be less noticeable than motor symptoms such as bradykinesia. Hyposmia is a commonly occurring symptom of Parkinson’s disease, reported in 80% of patients [21]. It is difficult, however, to determine whether the reported hyposmia in this study was due to the progression of Parkinson’s disease or chronic exposure to fire and smoke. Research has shown that chronic smoke and toxic substance exposure can lead to irreversible hyposmia [22]. In one study, 47.5% of 102 Chicago city firefighters had significantly low scores for a sense of smell test [23].
Conclusion
The purpose of this study is to improve our understanding of the relationship between toxin exposure in firefighters and risk of Parkinson’s disease. Firefighters have an increased risk for Parkinsonian symptoms as a result of the toxin exposures that are frequently present in fires. Our study showed that the number of years working as a firefighter, the number of days per week working, and the number of fires worked correlated with higher reports of Parkinsonian symptoms such as hyposmia, micrographia, and decreased walking pace. It is important that the scientific and firefighter community alike continue to develop studies aimed at determining the frequency of Parkinsonian symptoms in firefighters as well as the specific toxin exposures in order to potentially minimize the risk of developing PD.
Declarations
Consent for publication
The authors received written consent from Massachusetts firefighter Tim MacMillan who provided content for the background story.
Competing interests
The authors declare that they have no competing interests.
REFERENCES
- Ye S, Kim H, Jeong-Choi K. Parkinson's disease among firefighter: A focused review on the potential effects of exposure to toxic chemicals at the fire scene. Korean J Biol Psychiatry. 2017;24(1):19-25.
- Downward E, Pool JJ. How Common is Parkinson's Disease?: Parkinson's Statistics. 2019.
- Maetzler W, Liepelt I, Berg D. Progression of Parkinson’s disease in the clinical phase: potential markers. Lancet Neurol. 2009;8(12):1158–1171.
- Murphy B. Firefighters may have increased risk of developing Parkinson's Disease. 2019
- Caudle WM, Guillot TS, Lazo CR, et al. Industrial toxicants and Parkinson's disease. Neurotoxicology. 2012;33(2):178–188.
- Coon S, Stark A, Peterson E, et al. Whole-body lifetime occupational lead exposure and risk of Parkinson's disease. Environ Health Perspect. 2006;114(12):1872–1876.
- Baumeister S, Schepmann D, Wünsch B. Synthesis and receptor binding of thiophene bioisosteres of potent GluN2B ligands with a benzo[7]annulene-scaffold. Med Chem Comm. 2019;10(2):315-325.
- Konstandi M, Harkitis P, Thermos K, et al. Modification of inherent and drug-induced dopaminergic activity after exposure to benzo(alpha)pyrene. Neurotoxicology. 2007;28(4):860-867.
- Abrard S, Bertrand M, De Valence T, et al. French firefighters exposure to Benzo[a]pyrene after simulated structure fires. Int J Hyg Environ Health. 2019;222(1):84-88.
- Darnerud PO, Eriksen GS, Johannesson T, et al. Polybrominated diphenyl ethers: Occurrence, dietary exposure, and toxicology. Environ Health Perspect. 2001;109 Suppl 1:49–68.
- Hu CY, Fang Y, Li FL, et al. Association between ambient air pollution and Parkinson's disease: Systematic review and meta-analysis. Environ Res. 2019;168:448-459.
- Choi IS. Parkinsonism after carbon monoxide poisoning. Eur Neurol. 2002;48(1):30-33.
- Postuma RB, Montplaisir J. Predicting Parkinson’s disease-why, when, and how? Parkinsonism Relat Disord. 2009;15:S105–S109.
- Ouyang B, Baxter CS, Lam H-M, et al. Hypomethylation of dual specificity phosphatase 22 promoter correlates with duration of service in firefighters and is inducible by low-dose benzo[a]pyrene. J Occup Environ Med. 2012;54(7):774–780.
- Fires. Boston Fire Historical Society Official Website. 2020.
- Marusiak J, Kisiel-Sajewicz K, Jaskólska A, et al. Higher muscle passive stiffness in parkinson's disease patients than in controls measured by myotonometry. Arch Phys Med Rehabil. 2010;91(5):800-802.
- Park H, Park J, Lin S-H, et al. Assessment of Firefighters’ needs for personal protective equipment. Fash Text. 2014;1(1).
- Ball N, Teo WP, Chandra S, et al. Parkinson’s Disease and the Environment. Front Neurol. 2019;10:218.
- Desplats P, Patel P, Kosberg K, et al. Combined exposure to Maneb and Paraquat alters transcriptional regulation of neurogenesis-related genes in mice models of Parkinson’s disease. Mol Neurodegener. 2012;7:49.
- Sherer TB, Betarbet R, Testa CM, et al. Mechanism of toxicity in rotenone models of Parkinson’s disease. J Neurosci. 2003;23(34):10756-10764.
- Sveinbjornsdottir S. The clinical symptoms of Parkinson’s disease. J Neurochem. 2016;139:318-324.
- Crawford DZ, Souder E. "Smell disorders = danger." RN .1995;58(11):40-43. [Cross Ref]
- Manier J. Half of city firefighters losing sense of smell, new study finds. Chicago Tribune [Internet].


 symptoms.
symptoms.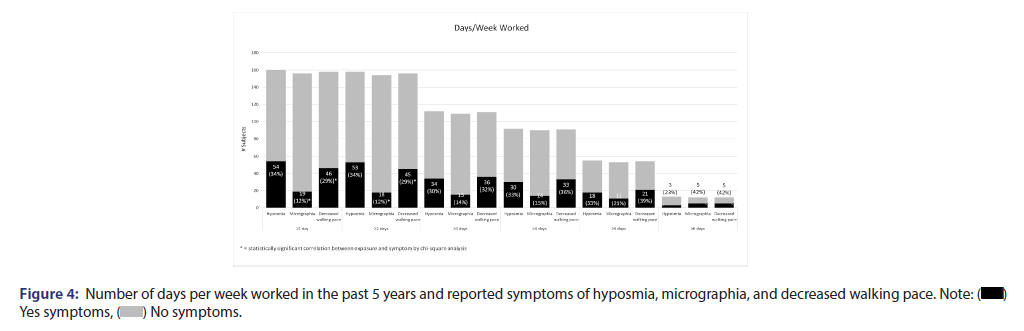
 Yes symptoms,
Yes symptoms,